
Tovah Ehrlich was 24 years old, feeling fine, and working as a receptionist as she began her last year at Queens College. In the home stretch of earning her degree, Tovah spent her free time painting, reading, or hanging out with friends — until halfway through her fall semester, when she started hearing a constant whooshing sound.
“It was November 2021,” says Tovah. “I remember hearing my pulse and a whooshing sound every time I’d bend over. I started getting migraines more frequently, and my vision would go blurry.” Those symptoms didn’t mesh well with her life as a college student and a receptionist in a busy office.
“It was a very loud environment, so it was bad,” Tovah says. “My migraines would be triggered by light, and I would take Excedrin to deal with it. I wasn’t sleeping very well. The pulsing noise would disrupt my sleep, and I’d have to put my palms on my temples and squeeze my head just to get the noise to stop. Only then could I try to sleep.”
Dr. Srikanth Boddu, the interventional neuroradiologist who diagnosed and treated Tovah at NewYork-Presbyterian Queens, has seen these symptoms time and again. “The symptoms she experienced were typical of idiopathic intracranial hypertension (IIH),” he says. “This is commonly known as pseudotumor cerebri, because its symptoms are similar to those of a brain tumor, without actually having a tumor."
IIH is a rare condition and its cause is still elusive, but it is associated with two findings. The first is an imbalance in cerebrospinal fluid (CSF), which surrounds the brain and spinal cord. The body continually produces and absorbs CSF, and when it produces too much or absorbs too little, the excess causes increased pressure within the skull. That pressure can cause migraines and blurry vision and can even lead to vision loss. The second finding is venous sinus stenosis — a narrowing of the veins in the brain, which results in reduced blood flow in the brain and increased intracranial pressure.
With her symptoms worsening, Tovah sought answers. “The catalyst for seeking help was that I generally wasn’t feeling myself and that I was gaining a lot of weight,” she says. “My mom did a lot of research and she was looking for help all over the place. She drove me to ENTs and allergists near her home in New Jersey.”
The doctors they saw couldn’t provide any answers, but there was a turning point in January 2022. “My mom saw a story featuring Dr. Boddu on the Weill Cornell website and sent it to me,” Tovah recalls. “I met with him, and he set up some tests to figure out what was going on. I had a lumbar puncture, eye exam, and CT scan done. Depending on the results, he’d send me for other tests. There was a lot to juggle; my mom had to come in from NJ to drive me. Since I was in school, I planned all my testing on days I didn’t have class. I was in and out of doctors’ offices for all of February. But all those appointments led to a confirmed IIH diagnosis — as well as the go-ahead to do the stenting procedure.”
“When diagnosing IIH, we have to rule out the presence of a tumor or any other condition in order to make the diagnosis,” says Dr. Boddu. “Once all the tests were done, and with Tovah’s scans in hand, we determined that the main cause of her IIH was venous sinus stenosis, which is easily treated with a minimally invasive procedure that my team and I specialize in: venous sinus stenting (VSS), which restores blood flow to the narrowed vein and remedies the intracranial pressure
“With a solution in sight, I felt relief, but it was hard on me,” recalls Tovah. “I was going to be a bridesmaid in a month and I didn’t want to be in recovery for that. So I waited to have the surgery, which was nerve-racking. But in the lead-up to the surgery, Dr. Boddu’s patience was helpful. I had a lot of questions, and he answered all of them. He was accommodating, too. I’m an Orthodox Jew, so I observe Shabbat on Friday and Saturday. Dr. Boddu rearranged his schedule and moved the surgery, which is typically on Fridays, to a Wednesday, which also necessitated moving surgical equipment around. I felt assured I was in good hands.”
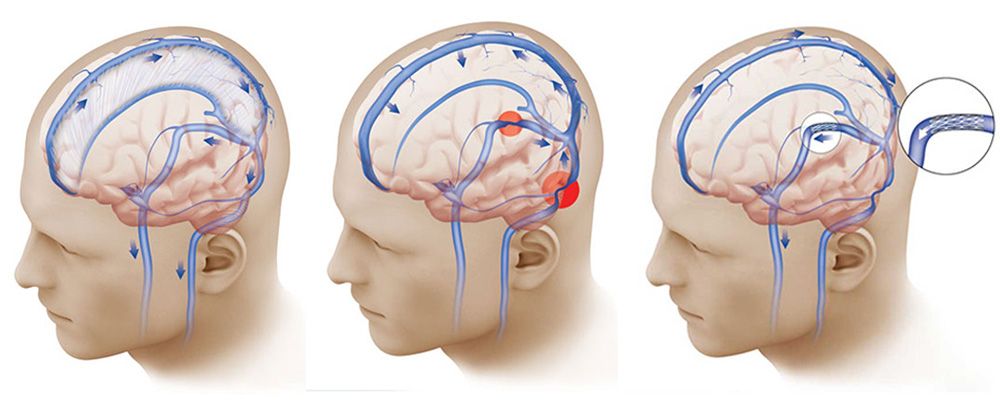
Normal pressure in the brain is maintained by a system that drains cerebrospinal fluid (left). In some people, a narrowing in those draining veins (red circles, center) interferes with that balance. A stent in those veins (right) can relieve the pressure.
As the day of surgery came closer, Tovah focused on the end result: finding peace. “It was driving me crazy. I hadn’t had silence for six months,” she says. “The migraines were getting more frequent. My sleep schedule was bad. I didn’t feel rested. Any reservations I had were overshadowed because I was so miserable. On the day of the surgery, I was nervous. I knew I’d be asleep for it, but once they put the IV in I got so nervous to the point where I cried a little bit. But throughout I was telling myself it would be over — and that I would be fine.”
“VSS is a very effective, advanced, minimally invasive method for treating venous sinus stenosis,” says Dr. Boddu. “We don’t have to drill through the skull. We just introduce a wide-bore needle in the patient’s upper thigh and thread a catheter to the narrowed vein. Once there, we deploy a stent, which expands the vein and restores blood flow to the area. Best of all, since the procedure is done without an incision or stiches, there’s less risk to the patient, and they’re able to recover very quickly.”
“After I woke up, I couldn’t hear the sound anymore,” Tovah recalls. “I took a picture of that moment. It was insane. They monitored me overnight and then I went home. My recovery was easy — I only had one or two headaches. But for weeks afterward I’d sit in silence at home and start crying because it was so quiet. Even now I’m thankful for the silence.”
Now, with the surgery behind her and her sociology degree in hand, Tovah has a greater appreciation for life. “When I first heard the whooshing, I thought the doctor would just tell me I had wax in my ear,” she says. “Never in a million years did I think I’d be having neurosurgery. I’m amazed that science and Dr. Boddu were able to help me.”
Tovah reports that the experience has changed her whole approach to life. “This all kicked me into gear,” she says. “Before the surgery I didn’t really think about my health. I didn’t pay attention to how I was feeling or what was going on. After the surgery, I got a reality check of certain changes I needed to make: healthy living and eating better. I realized I only have one life and that I had to take care of it.”
More about Venous Sinus Stenting | More about Dr. Boddu | More about IIH/Pseudotumor Cerebri