
When Shanon Lajoie moved to New Jersey in 2020, it was her third state in ten years. Shanon’s career had taken her from Connecticut to both coasts of Florida to New Jersey, with one constant and unwanted companion: the whooshing in her ears caused by pulsatile tinnitus. At 48, Shanon wanted nothing more than to enjoy the biking trails near her new home in peace – but peace was elusive after a decade of the whooshing. Today, thanks to Dr. Srikanth Boddu and the team at NewYork-Presbyterian and Weill Cornell Medicine, Shanon is living her life in quiet.
“I first started hearing the whooshing noises in 2011,” Shanon says. “It started a few months after I had an IUD put in. It was persistent throughout the day but seemed to get louder when it got really quiet, so going to sleep was trying. It got so bad that I’d have to press a vein on my neck to silence the noise. But walking around with a finger pressed into your neck is not a long-term solution, so I needed to see what I could do about it.”
“At this point, I’d seen eighteen doctors over ten years in four states,” she recalls. “I pretty much got the same answer from all of them: ‘It is what it is.’ Two separate ENTs administered a hearing test — I had to press my finger into the vein in my neck just so I could hear the sounds from the test to prove it wasn’t hearing-related tinnitus.” Shanon’s hearing was fine, but the doctors suggested sigmoid sinus surgery, in which a hole would be drilled in her skull behind one ear to then fill in so-called “missing bone.” It wouldn’t fix the problem, but she probably wouldn’t be able to hear the whooshing sound.
Shanon wanted a solution, not a hole in her head. When she mentioned this to Dr. Boddu, he said, “You didn’t get that done, right?!”

“Shanon was right: drilling a hole wouldn’t have fixed the root cause,” says Dr. Boddu. “Pulsatile tinnitus is a symptom, so you need to find what’s causing it. In many cases, it’s a narrowed vein, a condition called stenosis. The whooshing sound is in sync with the heartbeat — the heart pumps blood through the brain, and as it passes through that narrowed vein there is a disturbance in blood flow, resulting in the whooshing sound experienced by about five million people a year.”
By the time Shanon relocated to New Jersey in December 2020, she had done enough research to know that what she needed was an interventional neuroradiologist, a doctor with specialized training in procedures done under image guidance. (Diagnostic radiologists use scans to identify problems; interventional radiologists follow real-time imaging during treatment to resolve them.) In January 2022, after exhausting all potential doctors in New Jersey and Pennsylvania, Shanon started searching in New York. She came across an article from Weill Cornell Medicine Neurological Surgery about someone who had similar symptoms and had VSS surgery. A few weeks later, she saw her nineteenth and final doctor in the fifth state, after eleven long years: Dr. Boddu.
“We hear a lot of stories like Shanon’s, where doctors don’t know what the cause of the whooshing is,” says Dr. Boddu. “While very disheartening, it’s not surprising. Most doctors just don’t have the training or caseload to look for something like venous sinus stenosis. Because we specialize in its treatment, we see many of these cases.” Dr Boddu ordered magnetic resonance venography (MRV) for Shanon, and the scan clearly showed the narrowed vein causing the pulsatile tinnitus.
“I was flabbergasted,” recalls Shanon. “I brought similar scans with me from January 2017. I asked Dr. Boddu to bring them up next to the new ones to compare. They were identical. The radiologist I’d seen in 2017 had said my scans were unremarkable, that there were no problems. Every new doctor, in every state I’d been to since 2017, simply trusted that radiologist’s report and refused to look at the images. So when Dr. Boddu showed me the narrowed vein in my scans and told me he could fix it in the next few weeks, I couldn’t help but give him a hug.”
With a diagnosis in hand, Dr. Boddu told Shanon about a minimally invasive procedure called venous sinus stenting (VSS). “I was so grateful that Dr. Boddu not only identified the root cause but knew what the solution was within three minutes of looking at the MRV,” says Shanon. “He was wonderful. He was patient and kind, didn’t rush through our appointment, listened intently, and gave me as much time as I needed to process and understand what was happening next. Dr. Boddu made sure I was comfortable with the procedure and what recovery would look like.” Two and a half weeks later, Shanon had the VSS procedure.
“VSS, thankfully, is a far cry from drilling a hole in Shanon’s skull,” says Dr. Boddu. “It’s a minimally invasive procedure that starts with one needle in the upper leg to access the blood vessels. From there, we thread a tiny catheter starting in the femoral vein up to the affected vein in the brain, where we deploy a self-expanding stent. Once the stent is deployed, the narrowing is relieved, restoring healthy blood flow — reducing or completely eliminating the pulsatile tinnitus. Because the procedure is minimally invasive, patients are usually discharged the following day.”
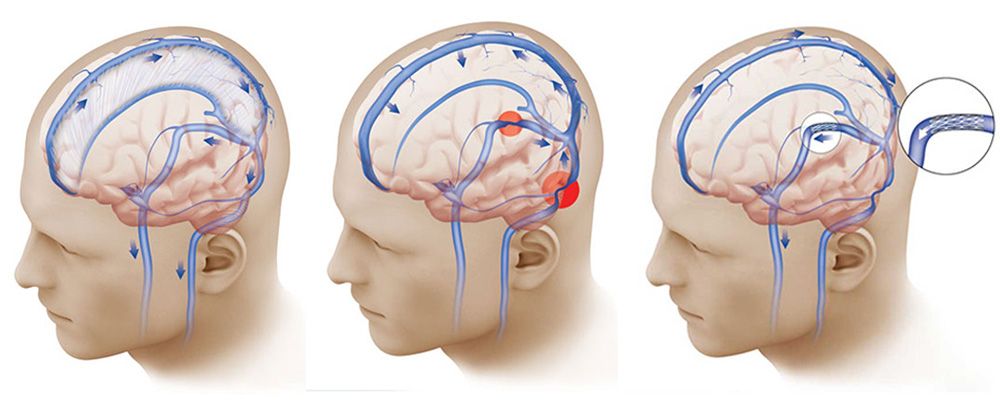
Normal pressure in the brain is maintained by a system that drains cerebrospinal fluid (left). In some people, a narrowing in those draining veins (red circles, center) interferes with that balance. A stent in those veins (right) can relieve the pressure.
“I was awake for the first portion,” recalls Shanon. “Once the catheter was in place, Dr. Boddu got the whole room quiet and asked if I could hear the whooshing. I said no and they put me under, and before I knew it I was in the recovery room.”
Dr. Boddu placed two stents to restore blood flow to Shanon’s narrowed vein. “When I woke up it was totally quiet; I couldn’t hear whooshing. After eleven years, it was gone!”

Shanon was discharged the following day. “I was sore in the groin area for a few days, but my recovery was smooth,” she says. “I went back to full functionality, and with no whooshing. I’m so happy I no longer have to hold my jugular to get to sleep.”
For anyone experiencing pulsatile tinnitus, Shanon has advice born of her decade of experience: “Keep being your own advocate and keep pushing,” she says. “With all the other doctors I saw, no one bothered to look at my scans. They just looked at the report from the original radiologist and blindly trusted it. I think that’s what bothers me the most. If anyone is reading this article and getting the same answers, keep looking to find someone who will look at the scans. Don’t accept ‘no,’ or ‘you’re going to have to live with it’ for an answer. You don’t. See an interventional neuroradiologist. Go to someone who specializes in it. Go to Weill Cornell Neurosurgery, because they can help you.”