The headache came from out of nowhere — the stabbing pain was like an ice pick in 17-year-old Aeris Clarkson’s head. “It just wouldn’t stop,” she recalls now. “It would be once a minute, or sometimes every fifteen seconds, a stabbing pain, again and again. I couldn’t do anything, it was so bad.” Her worried mom took her to the emergency room, where doctors told the teen that her headache was probably hormonal and gave her migraine medication. The pain started again in the car on the way home.
The next several months all went much the same way — relentless pain, an endless series of doctors and diagnoses, but no relief. “Nothing made a dent,” said Aeris, whose life had already been put on hold by the Covid-19 pandemic. The isolation and stress of 2020 was now compounded by the seemingly impossible quest to stop her pain. Doctors suggested she try different migraine drugs, acupuncture, ice packs, a chiropractor, nerve blocks, and massage therapy. Nothing worked except for the hot showers that would provide temporary relief – sometimes six showers a day, said Aeris’s mom, Jennifer.
“Aeris never complained, never got mad,” Jennifer said. “But she was in so much pain that she would just cry, and I didn’t know what to do. At one point she asked me, ‘am I just slowly dying?’ Imagine hearing your child ask that.”
Like any mom with a sick child, Jennifer was suffering as well, and she channeled her worry into action. As she lined up the endless series of appointments, she thought back to an earlier bout with headaches Aeris had had two years earlier. Those had been nothing like the new ice-pick headaches, and they had gone away, but Aeris had had an MRI done at the time. Jennifer said she’d never gotten any information about that scan, and since those earlier headaches had stopped she hadn’t worried about it. Now she was worried, and she called to see if that scan held any clues. Much to her surprise, the MRI results had never been reviewed by anyone.
"I realized that none of the doctors I was talking to were very experienced with pituitary issues. I did an Internet search for doctors who treat pituitary cysts, and the first name that came up was Dr. Theodore Schwartz.”
“When someone finally looked at the scan two years later, they told me it showed a Rathke cleft cyst,” Jennifer said. “But they also told me that it wouldn’t be the cause of her headaches, either then or now, and not to worry about it.” Jennifer's research confirmed that Rathke’s cleft cysts rarely cause symptoms, and she decided not to even tell Aeris about the finding. “She’s a worrier, and I didn’t want her to worry about something if it wasn’t a problem,” Jennifer said.
With multiple doctors saying the headaches were likely hormonal, Aeris saw a gynecologist, who ordered blood work to check hormone levels. The results were not typical at all — her prolactin level, which should have been under 25, was 106. She was referred to a neurologist, and an endocrinologist. Jennifer expanded her search for answers, contacting specialists and hospitals far from her home in Arlington, Texas. The answers were always the same: new doctors suggesting the same treatments that had already failed.
“It seemed that everyone just gave up,” said Aeris. “Nobody knew what to do for me.”
“When your child is in pain, every minute counts,” Jennifer said, “and this had been months. One place I called in October offered me a televisit appointment in January! I asked our local doctor about another MRI, and finally we had it done even though everyone said it wouldn’t help.” The new scan showed the same cyst, with no changes, and doctors again assured Aeris that it was not the source of her headaches. This time Jennifer was not convinced.

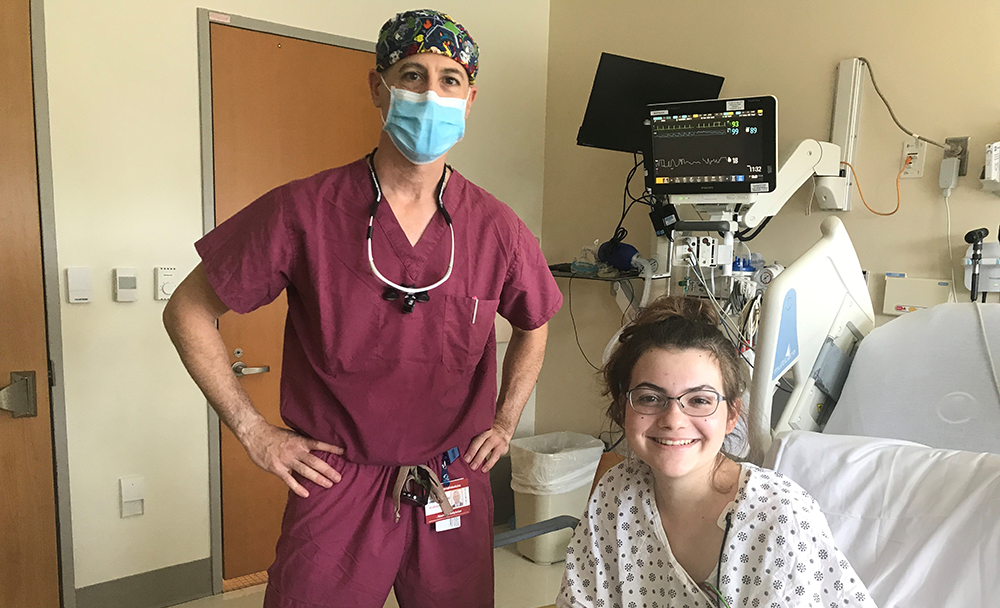
Aeris with Dr. Schwartz
“All the research I did was suggesting that the cyst could be the cause of the headaches,” said Jennifer. “Doctors actually laughed in my face when I’d ask about it. But I realized that none of the doctors I was talking to were very experienced with pituitary issues. They would call another doctor who had maybe seen one such cyst in his whole life, but nobody was an expert. They would look at the hormone test and agree that yes, the prolactin level was ‘up there’ — but they always said that couldn’t be the cause of the pain. I did an Internet search for doctors who treat pituitary cysts, and the first name that came up was Dr. Theodore Schwartz at Weill Cornell Medicine in New York.”
That’s a long way from Arlington, but distance no longer mattered. She needed an expert, someone who had seen hundreds of pituitary patients and who would know what to do, and that certainly described Dr. Schwartz. His team also took Jennifer seriously, in a way that other doctors hadn’t.
“By noon that same day I had an email back from his office — I couldn’t believe it,” Jennifer marveled. “I uploaded the scans, and Dr. Schwartz said he thought there was a good likelihood that surgery could fix the problem.”
What followed was a blur of activity — surgery appointment made, Covid testing done, flights booked, all in a matter of days. “I first spoke to Dr. Schwartz on November 6 and we flew here on November 10,” Jennifer said. Aeris met with Dr. Schwartz and Dr. Jeffrey Greenfield, a specialist in pediatric neurosurgery. The two experts would perform the surgery together.
“An MRI scan can show a growth, but not necessarily what kind,” said Dr. Greenfield. “When I looked at the scan I wasn’t convinced it was a Rathke cleft cyst, but from the image it’s impossible to tell. The symptoms Aeris was having certainly suggested that it might be a tumor, but as I told Jennifer, we just have to go in, and when we get there we’ll see what it is.”
“The MRI scan images were a bit ambiguous,” said Dr. Schwartz. “There was clearly a mass in her pituitary and we were leaning towards a Rathke cleft cyst but there was a good possibility it might be a tumor as well. If it really were a cyst we could probably drain it, and if it were a tumor we’d want to excise it completely. Either way, Aeris was a good candidate for a minimally invasive endonasal surgery, in which we navigate into the skull base through the nostrils, and don’t disrupt healthy brain tissue. That minimally invasive approach doesn’t even leave a scar, and the recovery time is quick. Either way, I was pretty sure if we removed this mass her headaches would get better and that was really the primary goal of the surgery since she had been suffering for so long.”
“I’ve been thoroughly amazed by this experience. What a wonderful environment this is. Everyone seems genuinely happy to be here, everyone has been so incredibly caring.”
Aeris and Jennifer needed to quarantine after arriving in New York from Texas, and Dr. Schwartz and Dr. Greenfield performed the surgery as soon as they were cleared. What the neurosurgeons found was not a cyst but a tumor — a prolactinoma, which had been responsible for both the elevated prolactin and the headaches. In an three-hour endonasal procedure, the surgical team removed the tumor. When Aeris awoke after surgery, the head pain was gone.
“It was such a relief not to feel that pain,” Aeris exclaimed. “I called my dad first, then started texting my friends. Everyone had been really sympathetic and supportive, but nobody really understood how hard it had been.”

Aeris with her mom, Jennifer
“I hadn’t seen a smile on my daughter’s face for months,” said Jennifer. The relief was palpable — the long journey was over.
Less than 48 hours after the surgery Dr. Schwartz was giving Aeris and Jennifer instructions about leaving the hospital, and mother and daughter were singing the praises of the NewYork-Presbyterian and Weill Cornell teams.
“I’ve been thoroughly amazed by this experience,” said Jennifer. “What a wonderful environment this is. Everyone seems genuinely happy to be here, everyone has been so incredibly caring.”
Looking back on the experience, Aeris says only that she hopes nobody else ever has to go through what she did. Dr. Schwartz echoed Jennifer’s thoughts about finding an expert: “Doctors who don’t see a lot of pituitary tumors simply don’t have the experience to know what these growths can do,” he noted. “The endocrine system is so complex, and the pituitary gland so powerful, that it takes years of working with them to recognize the signs. I’m so glad Dr. Greenfield and I were able to help Aeris and get her back to being a normal, healthy teenager.”
More about Rathke cleft cyst
More about prolactinoma
More about Dr. Theodore Schwartz
More about Dr. Jeffrey Greenfield
See also: Amanda Woerner patient story